When an ischemic stroke happens, every minute feels like a race against time to save the brain because it’s losing vital blood flow [4]. I’m Dr. Saher Arour, and I want to address a common question: how is a blood clot removed from the brain without open surgery? For some patients, the answer is mechanical thrombectomy: a procedure that uses a catheter and a device to help restore circulation[1]. My goal is to explain what this treatment involves, who might be a candidate, and what families can anticipate during this difficult time
- How physicians use catheters to reach the brain’s arteries.
- The imaging is used to identify patients who may qualify for treatment.
- The devices used to remove the obstruction.
- What families should expect after the procedure.
Table of Contents
What Mechanical Thrombectomy Is in Plain Language
Mechanical thrombectomy is a minimally invasive catheter-based procedure used to remove a blood clot in selected ischemic stroke patients [1]. In the clinical setting, we use this approach to reach the blocked artery directly through the vascular system rather than opening the skull. And the point is simple: quickly reopen blood flow in the right patient without open brain surgery. What matters to you here is that we can save time and minimize the physical toll on the body, allowing us to focus entirely on safely rescuing the brain
Why This Procedure Exists: The Problem It Solves
In my practice, I often explain to patients that a stroke can behave like a blockage in the brain’s arterial network. When a major artery is blocked, the brain tissue downstream begins to suffer from a lack of oxygen. Mechanical thrombectomy was developed for eligible patients with large-vessel occlusion, especially when rapid clot removal may improve the chance of preserving function [2].
What Happens During an Ischemic Stroke Caused by a Large-Vessel Occlusion?
Mechanical thrombectomy is used for eligible patients with acute ischemic stroke caused by a large-vessel occlusion, often referred to as an LVO [2]. An LVO occurs when a clot obstructs one of the major arteries supplying blood to the brain. This case is serious because these vessels supply blood to large areas of brain tissue. Without rapid treatment, the chance of long-term disability can increase.
The Evidence: What the Research Shows
For patients and families, the key message from the research is straightforward: endovascular thrombectomy improves functional outcomes in selected patients with acute ischemic stroke caused by large-vessel occlusion [5]. Clinical recommendations continue to support rapid evaluation and treatment because the benefit is time-dependent, and the goal is to treat as many eligible patients as possible as quickly as possible [4].
Step by Step: How the Procedure Works
Understanding the procedural flow can make the experience less intimidating for families waiting in the hospital. In the emergency room, time moves quickly, but I always assure families that this pace is built on absolute precision, not just time-saving. So we do not rush; instead, we follow a carefully rehearsed plan driven entirely by real-time imaging.
Step 1: Rapid Imaging to Confirm Eligibility
Once a patient arrives, the process begins. Brain imaging is performed as quickly as possible, and for patients who may otherwise qualify for thrombectomy, a noninvasive intracranial vascular study is recommended during the initial imaging evaluation [4]. In simple terms, this means we use advanced scanners to examine the blood vessels inside the head from the outside, safely and without making any incisions. In selected patients within 6 to 24 hours of the last known well, CT perfusion or diffusion-weighted MRI, with or without perfusion, helps guide treatment selection [4]. These images help us identify the “penumbra”. I often describe this area to people as our “window of hope,” because it represents brain tissue at risk that may still be saved if blood flow is restored in time.
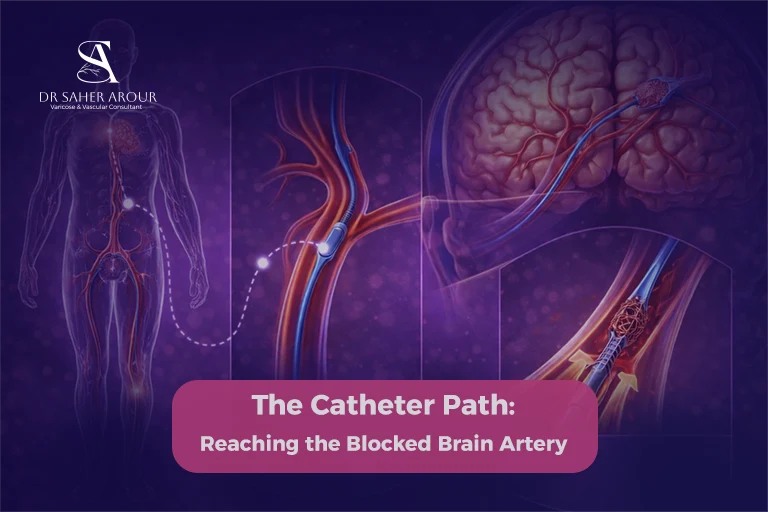
Step 2: Arterial Access: Entering Through the Wrist or Groin
To begin the procedure, we must gain access to the arterial system. In practice, doctors most often thread a catheter through an artery in the groin to reach the blocked artery in the brain [2]. Wrist (radial) access can be used as an alternative in selected cases, but the groin remains the usual route [7]. Once access is established, a sheath is placed to act as a gateway for the catheters that will travel toward the brain.
Step 3: Navigating to the Brain Artery
Using real-time X-ray guidance known as fluoroscopy, I carefully navigate the catheter through the arterial system toward the blocked artery in the brain. For patients, the important point is that this step is performed under imaging guidance so the team can reach the blockage as directly and safely as possible.
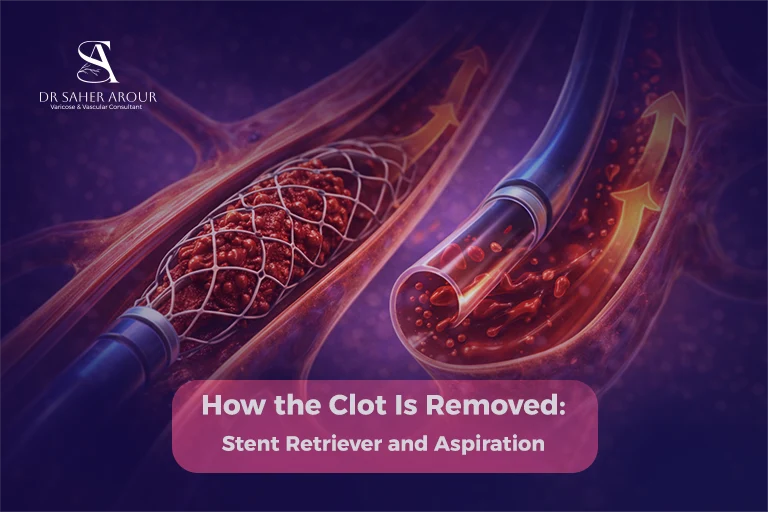
Step 4: Removing the Clot
Once we reach the blockage, the actual removal begins. And this is typically achieved using stent retrievers, aspiration catheters, or a combination of both techniques [2]. A stent retriever is a wire-cage device that opens and grabs the clot, while aspiration uses controlled suction to remove it [2]. For more information on the critical timing of these interventions, you can read our complete guide to brain stroke and the golden window for treatment.
Step 5: The Immediate Aftermath
After the clot is removed, the focus shifts immediately to close monitoring. In patients who undergo mechanical thrombectomy, it is reasonable to maintain blood pressure at or below 180/105 during and for 24 hours after the procedure [4]. The team also watches for complications and begins planning the next phase of care, including recovery needs [2].
Who Qualifies for Mechanical Thrombectomy?
Not every stroke patient is a candidate for this procedure. Selection depends on timing, imaging, the location of the blockage, and the patient’s overall clinical picture.
Standard Eligibility Criteria
When I’m asked why this intervention isn’t performed for every stroke patient, I explain that the most important goal is to ensure absolute safety while achieving a good recovery as quickly as possible. In the classic guideline-supported group treated within 6 hours, the criteria include prestroke mRS score 0 to 1, causative occlusion of the ICA or proximal MCA (M1), age 18 years or older, NIHSS score of 6 or higher, ASPECTS of 6 or higher, and treatment can be initiated with groin puncture within 6 hours of symptom onset [4]. While these medical terms and numbers may sound overwhelming right now, they are simply safety checklists we use to confirm that the brain tissue is healthy enough to benefit from the procedure without added risk.
Extended Window (Up to 24 Hours)
Historically, the treatment window was narrower. Current guidance recommends performing mechanical thrombectomy within 16 hours. It’s reasonable to consider up to 24 hours in selected patients with acute ischemic stroke, large-vessel occlusion in the anterior circulation, and advanced imaging features that meet DAWN or DEFUSE 3-style eligibility criteria [4]. This is why rapid imaging remains so important, even when a patient arrives later.
What Makes the Physician’s Experience Critical
The complexity of navigating the brain’s vascular system underscores the importance of the medical team’s experience. Higher operator experience has been associated with shorter procedural duration and better reperfusion, which is one reason operator experience matters clinically [3].
The Learning Curve Is Real and Steep
The medical literature supports the existence of a learning curve in performing mechanical thrombectomy, and cumulative experience can improve procedural performance [6]. At the same time, the exact steepness of that learning curve remains debated, so it is safer to say that experience matters rather than to overstate how quickly mastery is achieved [6]. For patients, that usually means the procedure is best delivered in centers and teams that perform it regularly.
Dr. Saher Arour’s Approach
When I sit down with a family to discuss this procedure, I focus on being fully transparent, of course, alongside clinical precision and patient safety. Because I know that every case is unique, I believe that the discussion should stay focused on timing, imaging findings, and the safest next step for the individual patient.
Recovery After Mechanical Thrombectomy: What to Expect
The end of the procedure is only the start of the recovery phase. Recovery varies significantly between individuals, and early care includes close monitoring for complications, preventing another stroke, and planning rehabilitation [2]. Families often want a fixed timeline, but recovery usually unfolds step by step and depends on the severity of the stroke and the patient’s condition afterward.
FAQ Section
Is mechanical thrombectomy a type of open brain surgery?
No, it is a minimally invasive procedure. Doctors use a catheter inserted through an artery to reach the blockage without opening the skull [1].
How long does the procedure typically take?
The duration varies from one patient to another. What matters most is that treatment and evaluation happen as quickly as possible, and greater operator experience has been associated with shorter procedural duration [3].
Can I receive both “clot-busting” medication and a thrombectomy?
Yes, if you are eligible. Patients eligible for IV alteplase should receive it, even if mechanical thrombectomy is being considered, and the thrombectomy evaluation should occur promptly at the same time [4].
References
[1] Top 10 Things to Know from the 2026 AHA/ASA Acute Ischemic Stroke Guideline
[2] Ischemic Stroke (Clots)
[3] Effect of Operator’s Experience on Proficiency in Mechanical Thrombectomy: A Multicenter Study
[4] 2019 Update to the 2018 Guidelines for the Early Management of Acute Ischemic Stroke
[5] Endovascular Therapy in Patients With Acute Ischemic Stroke From Large Vessel Occlusion: A Focused Update
[6] The Learning Curve in Mechanical Thrombectomy for Acute Ischemic Stroke
[7] Transradial Versus Transfemoral Access for Mechanical Thrombectomy: A Systematic Review and Meta-Analysis
